Monika Macejevska1, Jonas Lauraitis1, Jūratė Grigaitienė1,2
1Vilnius University Hospital Santaros Klinikos, Center of Dermatovenereology, Vilnius, Lithuania
2Vilnius University Faculty of Medicine, Institute of Clinical Medicine, Clinic of Chest Diseases, Dermatovenereology and Allergology, Center of Dermatovenereology, Vilnius, Lithuania
Abstract
Background. Crusted scabies is rare, highly contagious parasitic infestation caused by human mite Sarcoptes scabiei var. hominis and predominantly manifesting in immunocompromised patients. Due to insidious beginning, misdiagnosis is likely which may result in an outbreak of the infection. In countries where oral ivermectin is unavailable, treatment of crusted scabies presents a challenge.
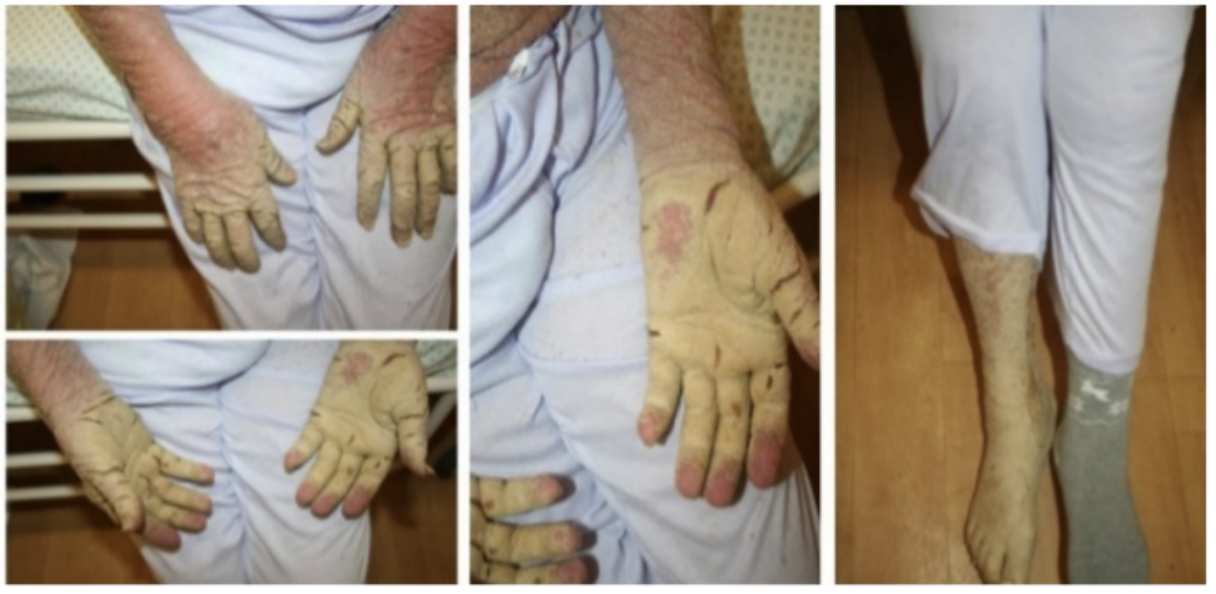
Case report. An 84-year-old immobile female patient with underlying malignancy was diagnosed with crusted scabies and successfully treated with keratolytic agents, surgical removal of crusts, permethrin cream, followed by daily applications of benzyl benzoate solution. Patient’s condition improved markedly after 14 days of treatment. However, 9 family members and part of medical staff became infected.
Conclusions: a combination of keratolytic agents, surgical removal of infected masses and topical scabicidal medications is equally effective treatment method for crusted scabies.
Keywords: scabies, crusted scabies, keratolytic, sulphur, surgical removal.